Fred N Davis, MD, Diplomat, American Academy of Integrated Pain Management, Clinical Associate Professor, Michigan State University College of Human Medicine
You might be noticing the term “social determinants of health” more frequently in the healthcare literature. What’s behind this and why is it important? As healthcare continues to evolve, efforts are underway to provide value based, whole person care in an environment that is increasingly shifting towards bundled payments. This means we have to be efficient in allocating limited financial resources. Healthcare leaders are now looking at what constitutes health and all that determines it in a larger context.
The Centers of Disease Control and Prevention defines health as a state of complete physical, mental, and social well-being and not just the absence of sickness or frailty (WHO 1946). Scientists generally recognize five determinants that contribute to a person’s current state of health. These factors may be biological, socioeconomic, psychosocial, behavioral, or social in nature (CDC 2014).
- Biology and genetics. Examples: sex and age
- Individual behavior and lifestyle. Examples: alcohol use, injection drug use (needles), unprotected sex, using a seatbelt, and smoking.
- Social environment. Examples: degree of support from family or friends, education, discrimination, income, and gender.
- Physical environment. Examples: where a person lives, pollution, and crowding conditions.
- Health services. Examples: Access to quality health care and the care rendered
The following graphic illustrates how much each of these factors contributes to the health of an individual or population (Minnesota Department of Health).
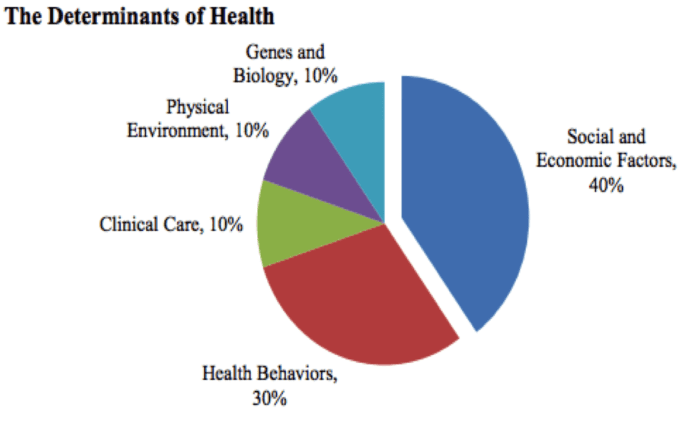
From this graphic, you can see that clinical care contributes only 10% to one’s health, and half of that is related to access alone rather that what care is actually provided. After practicing as a physician for over 30 years, it is humbling to learn that all of what we do in providing direct patient care only has a 5% impact on our patient’s health.
Looking at health and what constitutes healthcare, we need to shift our focus to the other determinants of health that may have a larger impact. This approach is being considered by the government in a new proposal from CMS (Medicare/Medicaid). In a recent speech, Health and Human Services (HHS) director Secretary Alex Azar said Medicaid may soon allow hospitals and health systems to directly pay for housing, healthy food, or other solutions for the “whole person.” Azar further explained that Center for Medicare and Medicaid Innovation officials are looking to move beyond existing efforts to partner with social services groups and try to manage social determinants of health as they see appropriate (Modern Healthcare Nov 2018).
If your organization is responsible for managing care for individuals and populations in this new environment (whether as a health plan, an ACO, a medical home, or a case rate-paid provider), interventions focused on providing health services alone have limited potential for improving health status. Rather, the most significant effect your organization can have on consumer health and consumer health care costs may be by developing new ways of tackling these other determinants of health.
Integrated team based care as taught at the Cummings Graduate Institute for Behavioral Health Studies prepares their students to understand the complex relationships between the physical body, lifestyle choices, and social determinants of health. They learn to look beyond a simple diagnosis and help treatment teams find innovative ways to address other factors that impact on the medical problem. In the coming months I will be speaking more about the topic of determinants of health. In the meantime, we can all be sensitive to these issues when seeing our patients.
- Preamble to the Constitution of the World Health Organization as adopted by the International Health Conference, N.Y., 19-22 June, 1946; signed on 22 July 1946 by the representatives of 61 States (Official Records of the World Health Organization, no. 2, p. 100) and entered into force on 7 April 1948.
- www.cdc.gov/nchhstp/socialdeterminants/definitions
- www.tcdailyplanet.net/race-and-health-inequities-report-legislature-reflects-daily-reality-clinics/
- www.modernhealthcare.com/article/20181114/NEWS/181119981





























